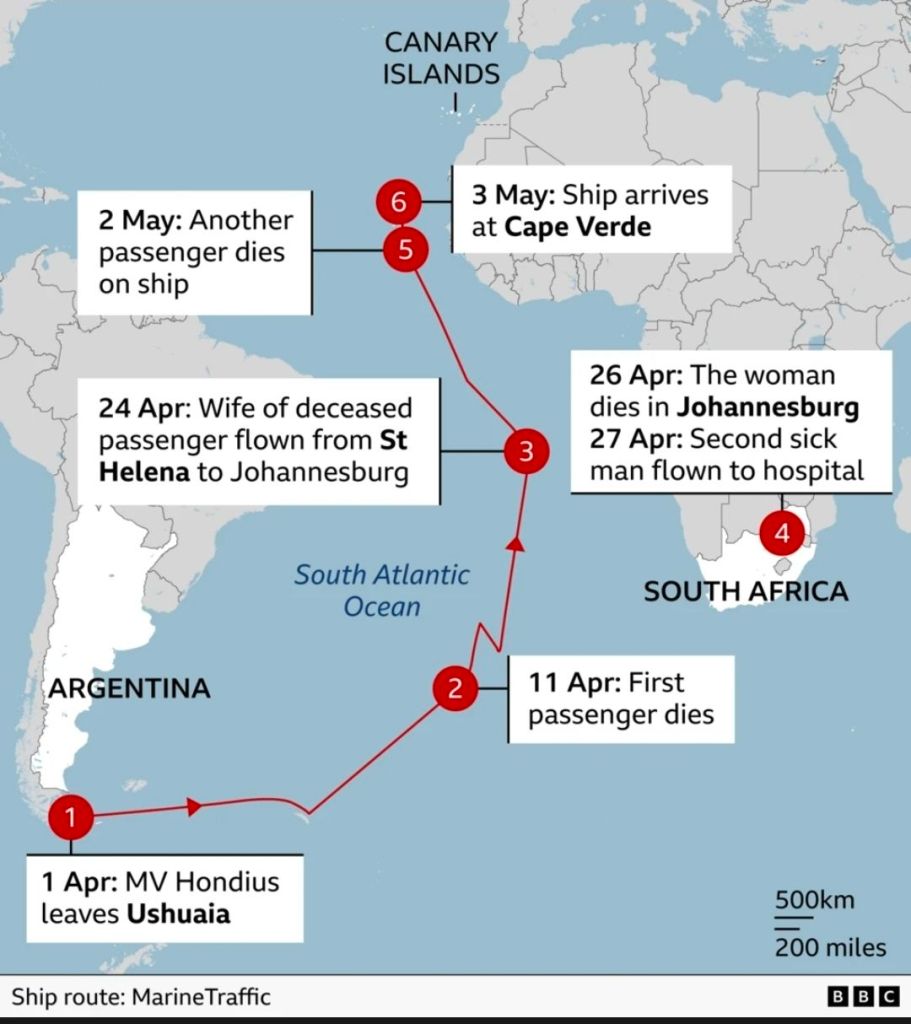
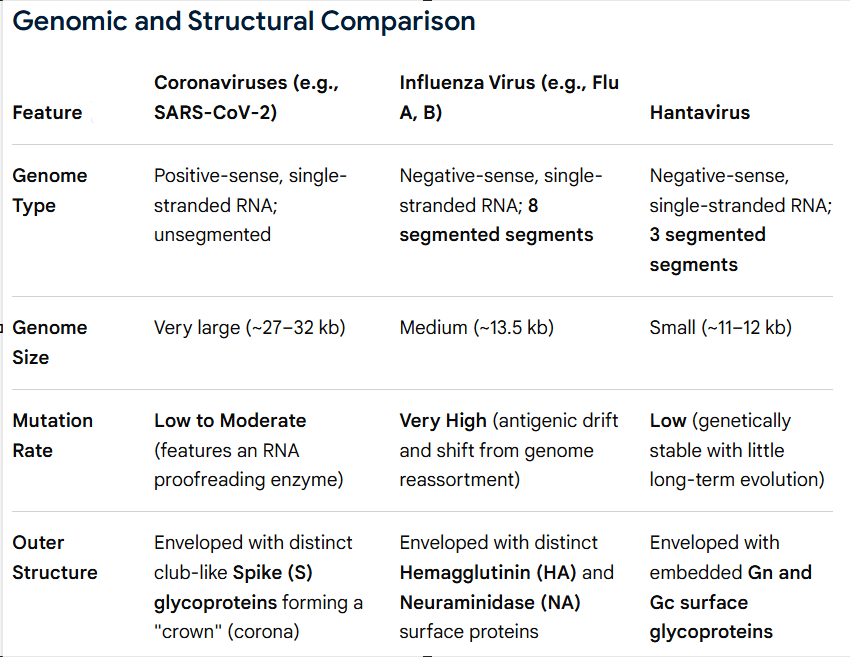
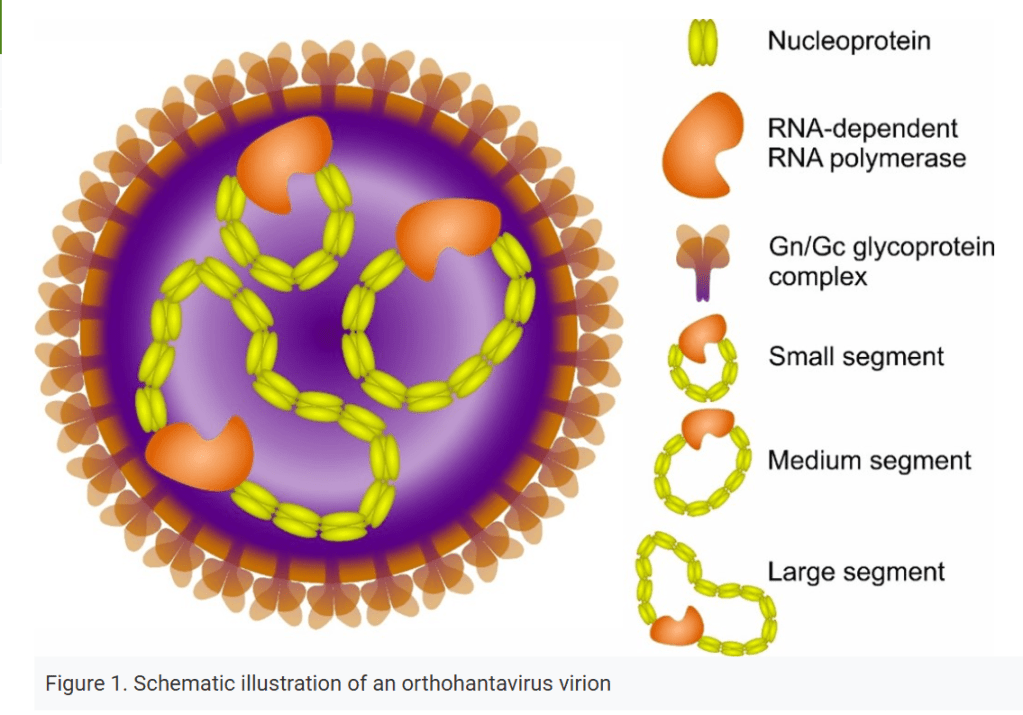
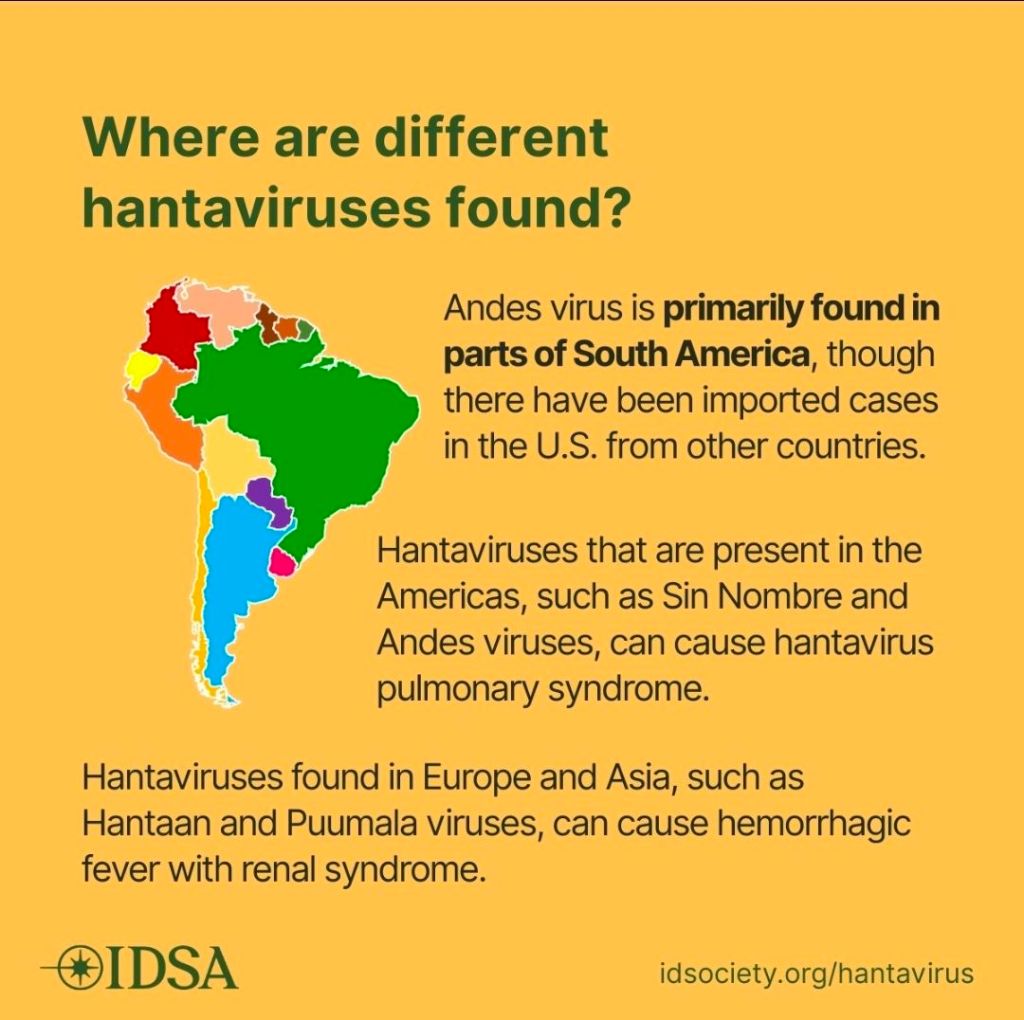
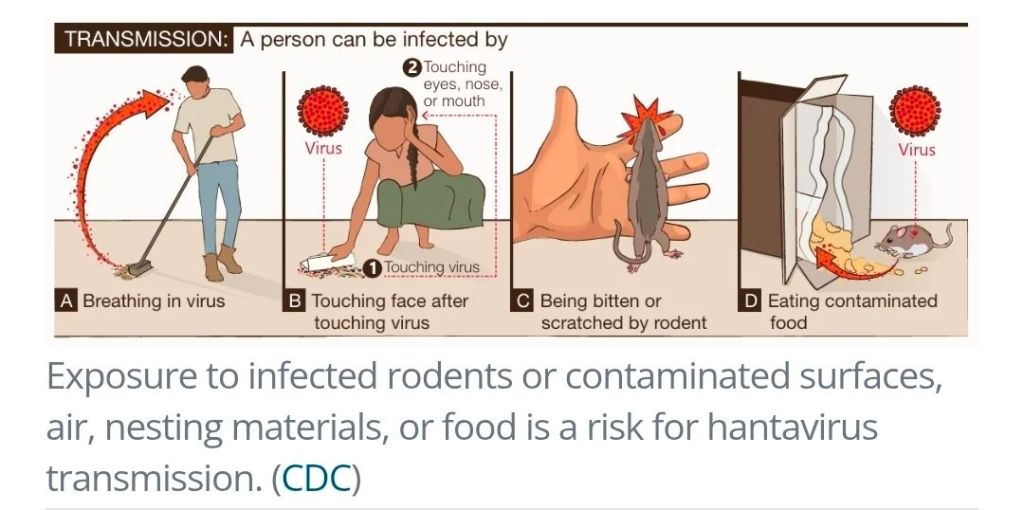
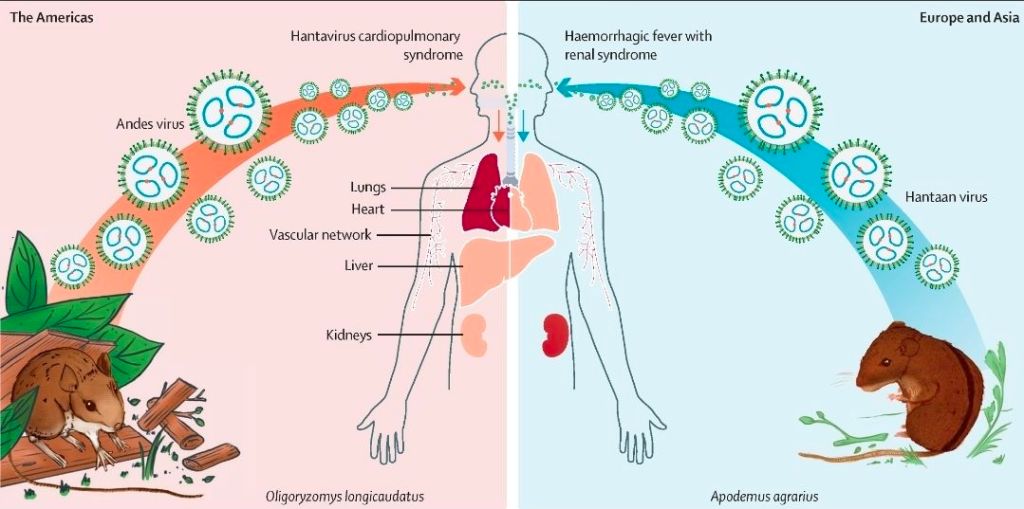
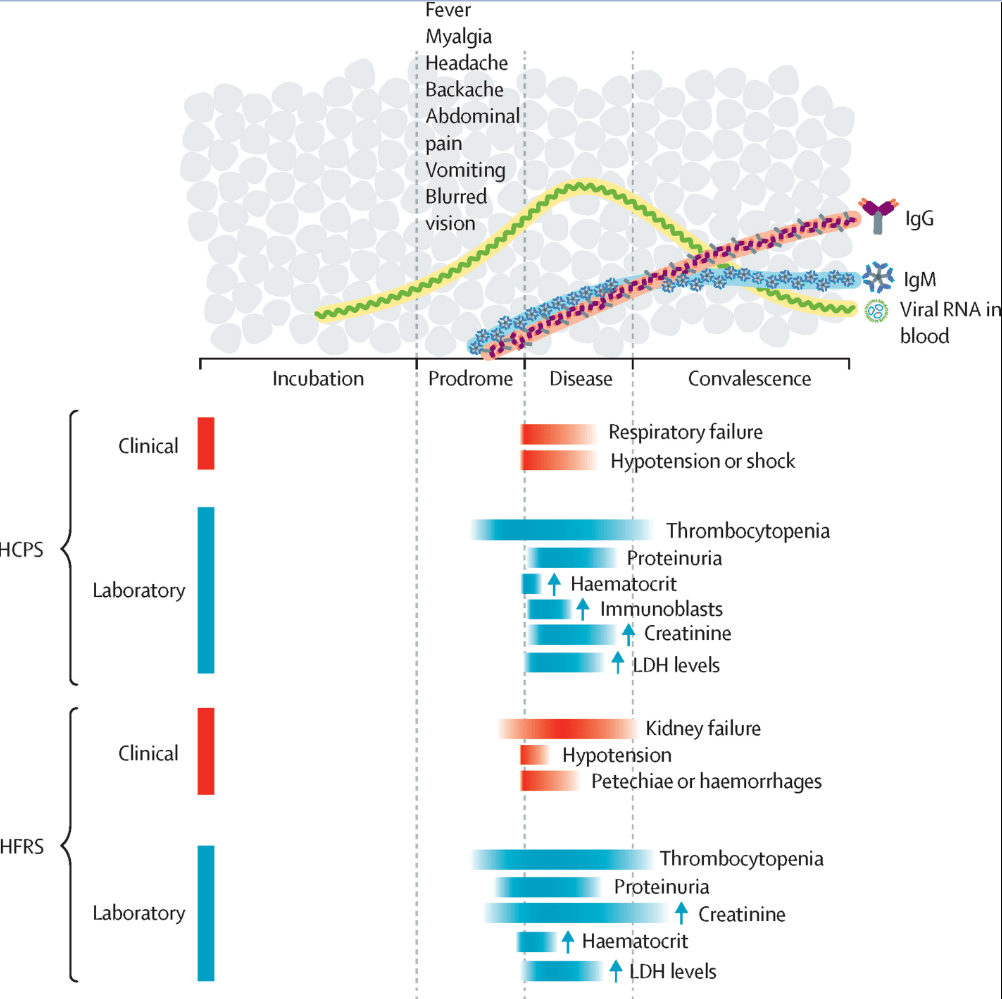
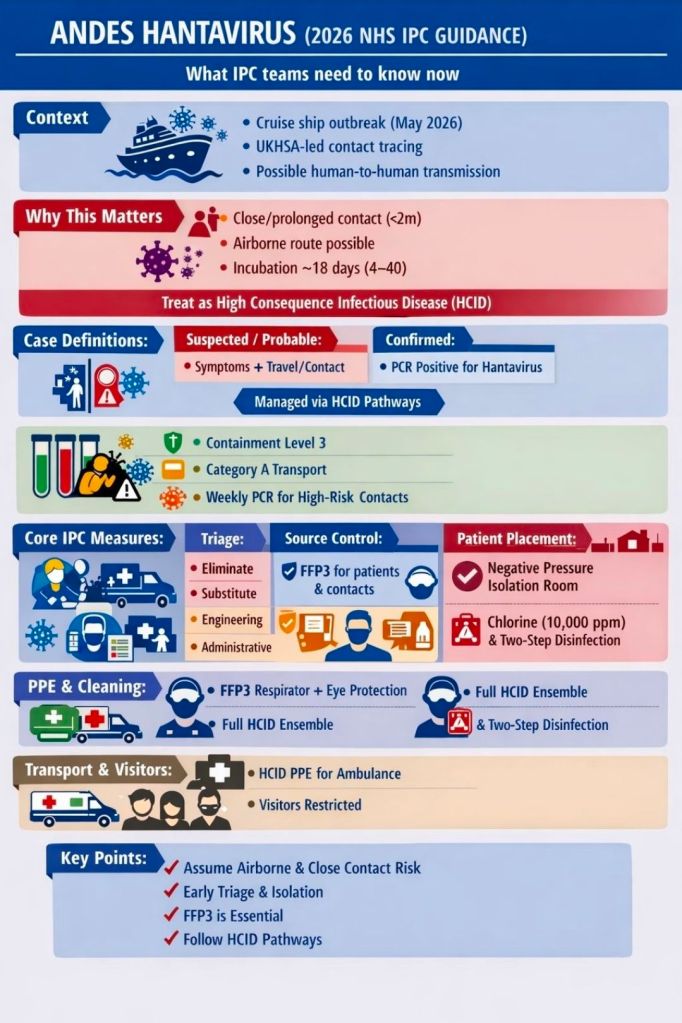
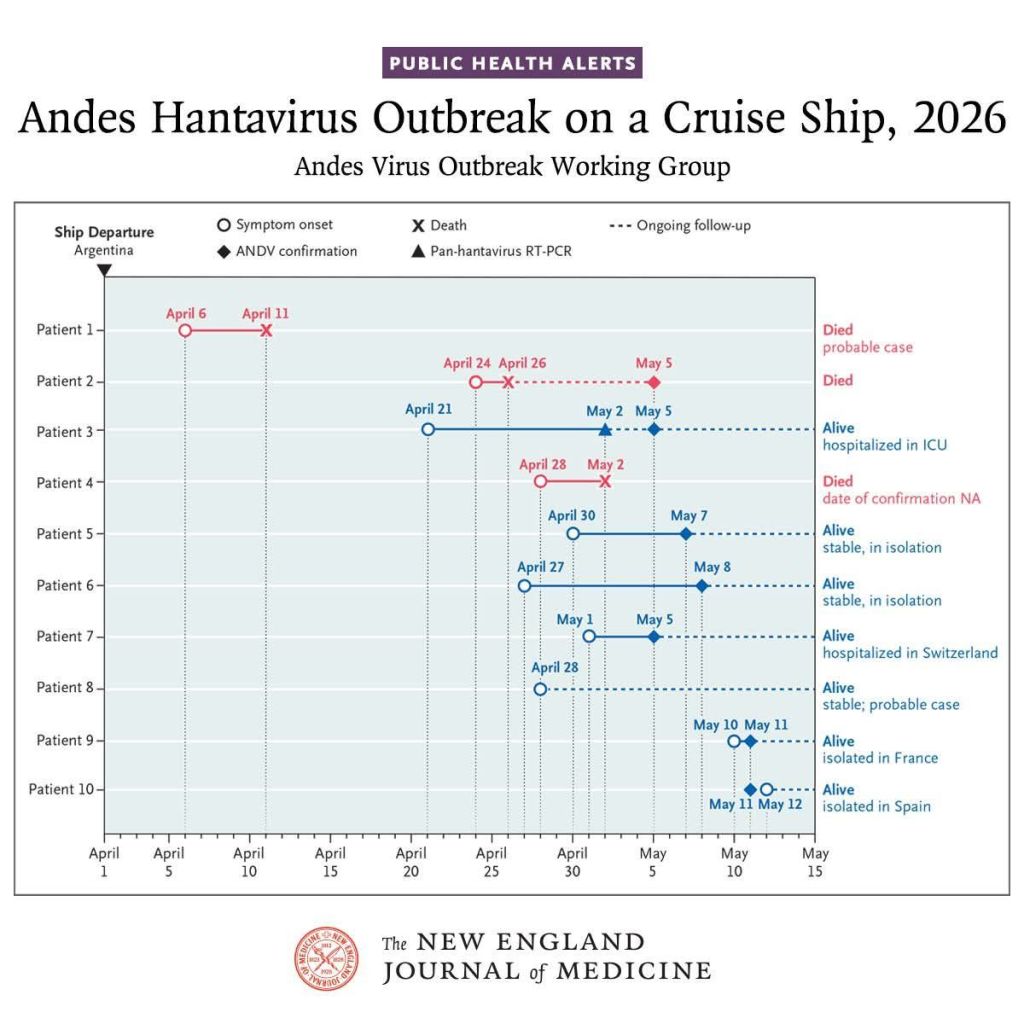
Cruise ships and cruise ship outbreaks have been in the news a lot this month. So much so, that I’ve already posted about the Hantavirus outbreak that was associated with a cruise ship in South America:
There have also been headlines, however, linked to 48 passengers displaying symptoms consistent with gastrointestinal illness, as well as one crew member, that has led to another cruise ship asking passengers to isolate.

https://www.bbc.co.uk/news/articles/cn5pe4yel1ko?app-referrer=deep-link
This second kind of cruise ship outbreak isn’t all that unusual, and I wonder if it would even have reached the headlines if it hadn’t happened during the same month as everyone was talking about Hantavirus. Cruise ships are mobile cities, with large numbers of people confined within a limit space, usually drawn from all over the world. Places where everyone is outside of their ‘normal’, eating different food together, spending time in close quarters with strangers, and sometimes reticent to lose holiday time if they start to feel unwell. That’s without throwing in sea sickness as an alternate reason for nausea and vomiting, which may mean people don’t realise they are ill with something infectious as early as they may do at home.
I’ve always sworn, for all of these reasons that I would never go on a cruise. I’ve spent way too many hours in lectures listening to outbreak stories related to ships, and yet, due to a birthday surprise, I went on my first ever cruise in 2025 and it surprised me, so I thought I would spend this week talking about a few of the reasons why, but first some outbreak context.
Multi-Year Outbreak Comparison (2019–2026)
According to historical Centres for Disease Control (CDC) data tracking of official gastrointestinal outbreaks across major cruise lines, the frequency of notable incidents varies dramatically by cruise line brand:
- Princess Cruises: Highest frequency with 14 outbreaks
- Holland America Line: 13 outbreaks
- Royal Caribbean International: 10 outbreaks
- Celebrity Cruises: 6 outbreaks
- Carnival Cruise Line: 2 outbreaks
- Disney Cruise Line: 1 outbreak
It’s worth noting, however, that different cruise lines not only have very different numbers and types of ships, with wildly different passengers numbers, but they also have very different passenger profiles. Some, like Virgin, host adult only cruises. Others, like Viking, serve older passenger demographics and undertake river cruising rather than ocean based cruising. Then you have lines like Disney, that focus on family centered cruising, and so will have a high proportion of families and young children as part of their passengers. Some cruises are also much longer than others, with cruises over six months becoming more common, and some cruise ships now consisting of passengers who have permanently brought cabins as their primary homes. All of which is to say, that numbers alone may not tell the whole story, and it is probably important to compare like with like.

NB Interestingly, as the recent Hantavirus outbreak did not impact 3% of passengers, I don’t know believe it would be reported via this system, and I suspect that they only manage US related outbreak numbers.
Outbreak Organisms (CDC list 2023 – 2026)
When you are training in microbiology, virology and infection prevention and control, you study A LOT of outbreak scenarios. Some of theses are almost always linked to outbreaks on cruise ships and/or navel carriers. Studies of re-supply and bringing in vegetables used for salads that took down 2/3 of the ship cohort with multiple organisms. I thought it might, thereofore, be interesting to look at the CDC data related to some recent outbreaks and see what the causative organisms actually are.
From 2023 – 2026 (to date) there were 54 reported outbreaks on the CDC website reaching the 3% of total passengers threshold. The causative organisms, where known, included:
- Norovirus
- Salmonella
- E. coli
- Combined Salmonella and E. coli
Now, I’ve previously posted about Norovirus, and how difficult it can be to control, especially the challenges of getting it out of environmental reservoirs (carpets, curtains, bedding) and so I’m not surprised that it is on the list.
I was interested to see how dominant norovirus was compared to other causes. When you look at the numbers it shows that norovirus really does seem to be as dominant as I was taught, with nearly 90% of outbreaks due to noro:
- Norovirus: 48 outbreaks
- E. coli: 4 outbreaks
- Salmonella: 1 outbreak
- Combined Salmonella and E. coli: 1 outbreak
Whilst noting that this feels like a lot of cases, it is also worth considering that the CDC states that cruise ship outbreaks account for just 1% of all reported norovirus cases globally. The other interesting thing is that the numbers seem to be pretty stable year on year, whereas out in the community I would expect there to be a significant rise in norovirus cases every 2 – 3 years, as strains change due to mutation, this doesn’t seem to be the case within the cruise data available.
Disney cruise line specific outbreaks
Having noted that Disney had only 1 outbreak listed recently on the CDC site, I thought I would investigate a little further. Disney Cruise Line has had two major officially documented gastrointestinal illness outbreaks that reached the CDC mandatory reporting threshold of 3% or more of passengers or crew, one in 2016 and one in 2002, each on a different ship:
Disney Wonder:
April–May 2016 (Official CDC Outbreak): During a 4-night Bahamian itinerary heading into a Panama Canal cruise, 131 of 2,680 passengers (4.89%) and 14 of 991 crew members (1.41%) fell ill with laboratory-confirmed norovirus.
Disney Magic:
November 2002 (Official CDC Outbreak): A total of 175 passengers and crew members out of 2713 passengers and ~950 crew, contracted norovirus during a Bahamian voyage. Disney temporarily pulled the ship from service for a week to break the infection cycle through a deep chemical sanitation.

Not all ships are equal
Something that struck me, is the outbreaks listed for Disney are to do with the two older ships in the Disney Cruise Line fleet, as they are both part of the Classic Class. This is interesting for 2 reasons:
- Is there an accumulation of outbreak risk due to age? Especially for organisms like norovirus which can be linked to environmental reservoirs
- The oldest 2 Disney Cruise Line ships were not a custom Disney build and so lack some of the specific design features that may support risk reduction on the newer ships
To aid with understanding this, it is noteworthy Disney has built a number of custom ships since the production of the Classic Class, and therefore have had the opportunity to include many more custom features in the later classes of ships.
The Classic Class – purchased by Disney but not a custom Disney design
- Disney Magic (1998) ~2700 passengers
- Disney Wonder (1999) ~ 2700 passengers
The Dream Class – commissioned by Disney for Disney
- Disney Dream (2011) ~4000 passengers
- Disney Fantasy (2012) ~4000 passengers
The Wish Class – commissioned by Disney for Disney
- Disney Wish (2022) ~4000 passengers
- Disney Treasure (2024) ~4000 passengers
- Disney Destiny (2025) ~4000 passengers
The Global Class – purchased by Disney but part built before acquisition
- Disney Adventure (2026) ~6700 passengers
One thing I didn’t realise, until I started to investigate this area more, is that cruise ships need to go into dry dock at least twice in every 5 year period by maritime law. Obviously mostly this is to do with safety, linked to the hull etc, but most cruise lines will use this opportunity to re-fit and manage any fittings and soft furnishings, which can aid with managing ongoing outbreak risk.

Why does Disney Cruise Line have to do things differently?
Full disclaimer here, I haven’t been on cruise lines with anyone else, but I have done a lot of talking to people and watching videos to enable some comparison, but my only first hand knowledge is from what I have experienced. I have only been on the Fantasy, and there are other classes of ships, obviously if Disney Cruise Line would like me to travel on them all to do an infection control audit, I’d be happy to, they wouldn’t even have to pay me.
I think, from my experience, one of the reasons that Disney Cruise Line is different, and has to be different, is because of the passenger demographic they serve. Their passenger number contain a huge amount of children under the age of ten. Children who may be shedding high viral loads, and carrying asymptomatic infection. Children who may also be too small to be able to communicate how they are feeling when symptoms come into play, and who may also not be compliant with hand and other hygiene practices, and are likely to be in close contact with others when playing etc. The ships are therefore at higher risk, potentially, than other cruise lines of having significant spread once a virus is onboard. It is also much harder to be able to isolate small children, and they are much more likely to need clinical support if they become unwell, which is a risk to the child and logistically complicated to manage. It is therefore much better to invest in steps to prevent infection spread.
What does Disney Cruise Line say they do to prevent the transmission of infectious disease?
Disney consistently ranks in the top five cleanest cruise lines globally. Their fleet frequently achieves perfect 100 scores during unannounced CDC sanitation inspections. They also have an advantage as they are an independent fleet, they don’t rent their ships out to others for events or specialist cruises, where they would have periods of time where they couldn’t control their risk. This allows them to maintain control of their fleet, what activities are undertaken, and ongoing control methods. The ships are also on the smaller size in terms of passenger numbers compared to some of the very large cruise ships managed by other companies (~2,700 to ~6,700 guests compared to ~5500 to ~7600 on some other lines).
Below is what Disney Cruise Line states about how they control their infection risks:
Key Quarantine and Isolation Protocols
- Mandatory Isolation: If you test positive for COVID-19 or another contagious illness during your cruise, you and your stateroom occupants will likely be required to isolate in your stateroom or a specially designated, safer area of the ship.
- Medical Evaluation: Shipboard medical centers are staffed with experienced doctors and nurses to provide care, and you may be required to quarantine at the sole discretion of the shipboard physician.
- Disembarkation/Evacuation: If necessary, you may be required to disembark early for medical reasons, which could occur in a foreign port.
- Pre-Boarding Screening: While pre-boarding testing is not always required, all guests must complete a mandatory health questionnaire before boarding, which includes screening for symptoms like fever, cough, vomiting, or diarrhea.
- Compliance: You are required to abide by all health safety protocols, which can change without notice, and failure to comply may result in denied boarding or forced disembarkation.
- Stateroom Support: If you are required to isolate, Disney provides necessary support, including food delivery and medical check-ins.
- Illness Prevention: The crew conducts extensive cleaning and sanitization of common areas and staterooms
Now, luckily for me, I didn’t experience any sickness onboard and so I can’t testify to the accuracy from all of these portrayals. I can, however, attest to many of other aspects, such as pre-screening, cleaning, and hand hygiene support.
Operational approaches
There were some brilliant operational choices that made me both happy and also surprised me. There were also some really simple design decisions, which now I’ve seen I don’t understand why they aren’t present everywhere. The best example of this was the way that plates on the buffet were stored upside down. This means that no one is in contact when taking a plate with the surface that someone else will then eat off. This is such a simple change but makes so much sense in terms of infection control I can’t believe I have neither thought about it myself or seen it elsewhere.

Other simple things included the fact that all cutlery was left fully wrapped, and so no one was touching the implements that anyone else was going to eat with. This fully enclosing, rather than just wrapping, is another easy way of prevention cross transmission routes, as asymptomatic, or even symptomatic excreters, are not in a position to pass on their organism to others. It also prevents deposition on cutlery from other routes, such as when people sneeze, effectively providing a protective barrier.

Self serve vs cast member led
Another key thing, on some ships, is that the buffet is served by cast members rather than self serve. This means that the food is kept behind screens and significantly lowers contamination risk. All main meals are served plated by cast members, which also reduces reduces the risk. Even self serve items, have guidance linked to risk reduction. For instance the fizzy drink dispensers advice people not to use reusable cups, so that the dispenser outlet does not risk re-contamination after someone has drunk from the cup.

Keeping hand hygiene easy
Something else, that is very prominent, is the emphasis placed on hand hygiene wherever you go onboard. Hand hygiene stations are conspicuously present with both adult and child height basins. Special sinks are also present in all the child specific areas that can help children with hand hygiene, as all they have to do is submerge their hands and the sink itself undertakes the agitation. This helps hygiene efficacy for children who younger or less engaged.
Multiple hand hygiene stations are available at the entrances to the buffet, and there are enough of them that no one should skip unintentionally because they haven’t seen them, or because people are off-put because of queues. Making hand hygiene easy and visible has been found to be key from healthcare studies, and I imagine cruise ships are no different.

Gatekeeping
At main dining room meals, in the evening, hand hygiene is actively enforced. As there are too many people entering the dining rooms at each sitting (as everyone eats at either early or late dining) Disney enforce hand hygiene by having crew members physically hand out hand sanitising wipes directly to each passenger as they enter the dining room. The same happens at the buffet at busy times. This is very different (from what I can tell) to other cruise lines and definitely contributes to risk reduction. Having these multiple points, every day, where hand hygiene is enforced really helps to impact the collective risk level onboard.

Bathrooms
Even the bathrooms pleased me, and not just because of the Mickey shaped mirrors. Having a feature that attracts people towards the sink does help with hand hygiene compliance, however. They also have signage on how to wash your hands by every sink, to encourage that it is done appropriately. Additionally, many have access to hand hygiene in areas after you have exited the bathroom door, to manage any exit contamination risk, as an additional option.

Domestic cleaning
Cleaning is obvious everywhere you go. I may have been the only person on that cruise who spent time photographing the cleaners trolley rather than the ‘big five’. All rooms got cleaned at least once a day, but in my experience many rooms got cleaned twice a day, as they get a morning clean and an evening turn down. Eating areas are also rotated and open at different times which allowed cleaning to be supported. Spending so much time auditing, I am often super aware of environmental grime, and no once was I brought out of the magic of being onboard by seeing anything that triggers my IPC brain.

Cleaning trolleys have freshly made up cleaning solution, alongside cleaning wipes. Fresh cloths and easy access to gloves. The level of cleaning we experienced was immaculate, and this does seem to align with the CDC audit scores.

Pre boarding
There are steps taken to reduce risk, however, before you even get on board. Disney Cruise Line requires all guests to complete a mandatory, online health questionnaire on the morning of embarkation, typically arriving via email between 5:00 a.m. and 6:00 a.m. The is pretty brief and asks a series of “Yes/No” questions regarding recent fever/respiratory symptoms, gastrointestinal issues, and pregnancy status (specifically for those 24 weeks or more). Although not infection related the pregnancy question is an interesting one and often catches people out. Disney, like many cruise lines, won’t let women sail if they are over 24 weeks pregnant. This appears to be standard across the industry because , if a medical emergency or preterm labour occurs, ships do not carry the specialized equipment or staff required to safely manage delivery or provide neonatal care for a premature infant.
If you reply in the positive to any question, other than the pregnancy question which is an immediate no board, then you will usually be reviewed prior to boarding and a risk assessment performed.
During cruising
If you develop symptoms of any kind, once you are onboard, there is support available from the medical team. It may be hard to distinguish between gastrointestinal symptoms and sea sickness, and everyone is encouraged to flag anything in order to ensure the right risk review is undertaken. If it is felt to be an infectious cause, passengers will be asked to isolate, and enhanced cleaning is undertaken.
Not only is hand hygiene reinforced during signage, by telling you not only how but when to wash your hands, it also clearly flags that you should contact medical support staff if you experience symptoms, and helpfully even flags what they are. All of this means that they are multiple contact points every day where passengers can access information that may be helpful in reducing infection risk (also, how clean are those tiles).

During excursions
Hand hygiene is also enforced after excursions before you get back onboard the ship. Alcohol gel dispensers are brought out by the crew, and cool towels, as well as water, are available to aid passengers stay cool and hydrated. I’m sure if you were in colder climes these would be aimed at warming you up.

Signage is also placed outside of disembarkation points that can help guide whether special measures may be needed or advised before you start on excursions. I think most people are more concerned with COVID still than norovirus, whereas I am very much concerned about diarrhoea and vomiting as part of my ship board experience.

Visible prioritisation
In general the communication of the need for hand hygiene is ubiquitous onboard. The signage below was part of the display in the lifts on the Fantasy. Embedding this guidance, and having it reinforced by cast members, means that for the most part everyone just complies without the need for prompting. I suppose it should be no shock that Disney do communication well, so much so I think there are some things we could learn in hospitals about how it is approached.

Design led solutions
The other area that healthcare could learn from is some of the design based solutions. We obviously have a lot of hands free options in healthcare but it was great to see these design points across the ship to minimise areas where hand contact is concentrated by needing to touch single points. A lot of thought has been given to pinch points in the system, and actions like manually supporting hand hygiene using wipes really also helps to address these.

Things I still can’t get over
Having talked about everything I loved, there is one thing that I don’t think I’ll ever get over, the people soup that are shared spa pools. The idea of sharing warm bubbling water with strangers and imagining our shared bacteria growing is something I can’t get passed. Also, I need to see the Pseudomonas testing certificates. This isn’t a Disney specific aversion, I just don’t think I can get my head around them anywhere. Nothing is perfect.

Where can I learn more?
I was taking on my cruise as a surprise, but Mummy and Mr Girlymicro has done a LOT of research before we want, so much so they even had to delete their YouTube histories so I wouldn’t notice. All lines have different risks, so I would advise doing some research to see which ones have risks that you are prepared to engage with. For me, I’m a Disney girl and I’m yet to see information from any other cruise line to temp me into doing something different. What can I say, I’m a convert to cruising, but only under a very specific set of parameters, and if Disney ever need infection control support, all they have to do is call me.
If you want to learn more, or check out your own cruise line of choice, the CDC website that contains a lot of info:
https://www.cdc.gov/vessel-sanitation/cruise-ship-outbreaks/index.html#
All opinions in this blog are my own