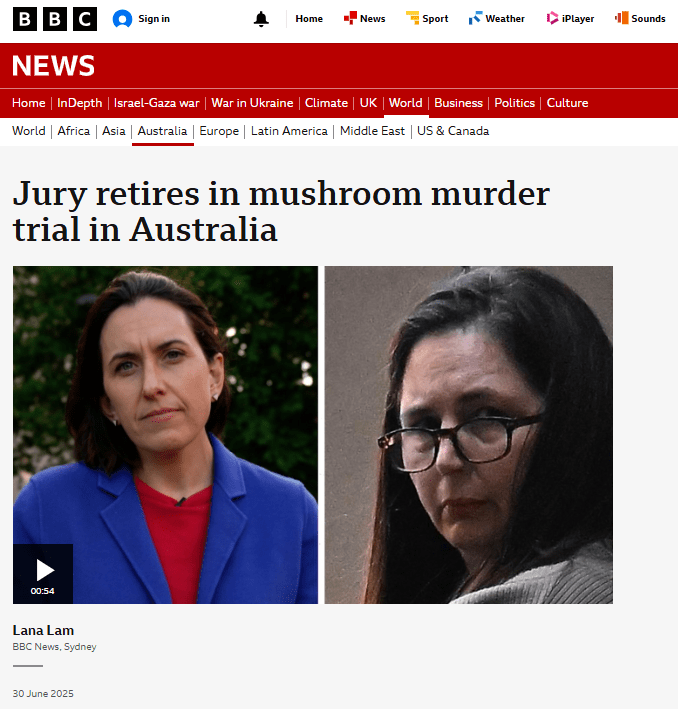
I’m so excited by this weeks guest blog post. I’m a massive murder mystery fan, and from Agatha Christie onwards there have been multiple books where mushrooms and mushroom toxins (mycotoxins) have been used, either deliberately or accidently, as a pivotal component of the plot. In recent months however, mycotoxins have been in the news in a real world sense, as the case of Erin Patterson has been heard and the jury are deliberating as I write. Erin Patterson is accused of 3 charges of murder, and one of attempted murder, linked to feeding guests a poisonous dish of Beef Wellington at a dinner party.
This led me to speak to my go to guy for mushroom (mycological) based questions. Sam is in love with all things shroom, and even has a mushroom foraging based Instagram. Who better to go to with a request to write a blog post on mycotoxins and to learn more about this intriguing topic?
Blog by Dr Sam Watkin
Hello Girlymicro blog readers! I’m Sam, a previous PhD student of Elaine’s with research focused on investigating trends in microbial dissemination in hospitals. I’m taking the blog astray from the world of IPC however with this post, and instead will focus in on one of my other interests. As people who know me have probably come to realise, I’m a big fan of mushroom foraging. There is something so rewarding to me about finding excellent edible mushrooms that you just can’t buy in shops and exploring the different flavours they can add to food. My partner had to put up with me having a Cauliflower fungus (Sparassis crispa) the size of a football in our freezer for well over a year. We would break bits off and make fantastic soups and stew bases with it – it has a really unique nutty flavour. More than just the pursuit of a free dinner though, I find it very enjoyable finding fungi that I haven’t seen before, or that are particularly rare. I imagine it is similar to the enjoyment a twitcher gets from sighting a rare bird, although mushrooms tend to stay put so there is less pressure on being constantly focussed. Having said that, searching for fungi does often devolve into a game of looking at the brown forest floor trying to spot the slightly-different-brown mushroom. More than once have I run over to a promising shade of brown or yellow, only to be disappointed by a frustratingly deceptive leaf. It is nevertheless a pursuit I thoroughly enjoy, despite the frequent soakings in rain showers and occasional run-ins with brambles.
One aspect of foraging (and indeed looking to identify fungi) is being aware of what ones you can eat and what ones are to be avoided. The old adage “All fungi are edible, some fungi are only edible once” absolutely holds true. While my professional life involves researching microbial transmission and how best to prevent infection, I am fascinated by the toxic nature of fungi. I did consider becoming a toxicologist in my teens, but rapidly realised that the amount of chemistry required was simply not my idea of joy. I do find it very interesting however how fungi are capable of producing some of the most unpleasant, and also strangest, toxins that can be found in the natural world (or at least I think so). So here I am going to run through a few of the fungi that I find most fascinating when it comes to their chemical makeup and the influence they have had on humans through history.
A fairytale classic – Amanita muscaria
Few fungi are more iconic than A. muscaria (known in English as the Fly Agaric). Their characteristic red caps and white flakes are often illustrated in children’s books and are probably what comes to mind when one pictures a ‘toadstool’. They are in every respect the archetypal fungus. This being said; however, you absolutely would not want to eat one. If someone were unfortunate enough to eat a specimen on A. muscaria, they would most likely experience a range of unpleasant neurological symptoms. Confusion, dizziness, ataxia, hallucinations, muscle twitching are often reported, as well as nausea and vomiting. In severe cases, a loss of consciousness and dangerous decreases in blood pressure can occur. These unpleasant effects are due to the makeup of alkaloids present in the fungus, with ibotenic acid and muscimol being predominantly responsible for these effects. Muscimol has a similar molecular structure to GABA-A – the most abundant inhibitory neurotransmitter in the human brain. Ingesting a chemical which mimics such an important neurotransmitter as part of your supper is unlikely to be good news. It acts as an agonist for GABA-A receptors, causing a reduction in the excitability of neurons, causing the range of neurological symptoms. Muscimol is by no means alone here however – A. muscaria also contains ibotenic acid which further acts as an agonist of a host of neurotransmitter receptors (for instance metabotropic glutamate receptors – another widespread neurotransmitter receptor class. Oh, and ibotenic acid is metabolically converted to muscimol in the body. More fun to go around!

It’s not only the alkaloid balance or popular culture appearance of A. muscaria that makes it interesting however – it has had significant historical and cultural influences. It has been traditionally consumed by shaman in northern Europe as a part of winter solstice celebrations. This is due to the intoxicating effects of consumption, where the experience was likened to flying. Part of the rituals would involve the fungi being collected while wearing ceremonial red robes. The fungi were also often fed to reindeer before ingestion to metabolise out some of the more toxic components, with the hallucinatory agents collected in the reindeer’s urine which was then consumed. I’ll pass. But, an association with winter and red robes, feelings of flying and reindeer… these rituals have indeed been credited as a potential origin of the popular imagery of Santa Claus. I guess everything must start somewhere!
An explosive pufferfish – Gyromitra esculenta
I find this to be one of the most fascinating fungi in existence. Partly fuelled by the fact that I still am yet to find this species growing wild (one day my persistence will pay off) and partly by how unique these fungi are both in shape, cultural perceptions and toxicity. Looking like mini brains, they can be found under pine trees on sandy soil in autumn (or so I’m told… maybe they are deliberately avoiding me). They are found in Europe and certain parts of North America, and are called False Morels due to their relation and similarity to the delicious Morels.
Despite being well known as a poisonous fungus their name would suggest otherwise, with “esculenta” being Latin for “edible”. And these fungi are indeed eaten in large quantities! When prepared correctly. As such, they have been likened to the pufferfish of the fungal world, which is quite the title! Appropriately prepared they are supposed to be a delicacy – I can’t speak from experience on this one, my adventures into free fungal food doesn’t quite stretch this far – however raw or improperly cooked they can be fatal. This toxicity is down to the presence of a volatile toxin called gyromitrin. When ingested, gyromitrin is metabolised to monomethyl hydrazine. This goes on to wreak havoc on a wide range of enzymes and processes, inhibiting cytochrome P450, amine oxidases and preventing the formation of pyridoxal 5-phosphate. This compound is a key cofactor in the synthesis of our old friend GABA. This causes a reduction of GABA present, preventing neuronal inhibition and causing to a prolonged excitatory state in the brain – almost the opposite of the effect seen in A. muscaria. This is still not good news however, with symptoms including severe gastrointestinal distress, kidney and liver damage and seizures and death in severe cases. Interestingly, the toxic metabolite produced here is used amongst other chemicals as a rocket propellant. I can’t but help imagine a future where we have spacecraft fuelled by fungi (albeit from a poisonous metabolite of a mycotoxin). Somehow, I doubt it.
Building up to it – Paxillus involutus
Following on from the theme of the last fungus, P. involutus is no stranger to gastronomic controversies. This very common, fairly non-descript fungus is a rather boring shade of brown (sorry if this is your favourite fungus!), although its cap does have a uniquely rolled-over rim (hence the imaginative English name – Brown Roll-Rim). It has historically been considered to be an edible mushroom, with many guidebooks simply stating that once cooked, it was safe to consume. Needless to say, these guidebooks are now firmly out of date and it is now recognised as a deadly poisonous fungus. Unlike the previous two fungi I’ve described here, this fungus does not contain any psychoactive alkaloids or toxic rocket fuel precursors. Instead, this species contains some rather unpleasant irritants which, upon consumption of raw specimens, result in severe gastroenteritis. These toxins however are degraded on heating, hence why it used to be considered edible after cooking. No, the real toxins are much more sinister in this fungus.
True to the weird nature of fungi, this species rebels against the “only edible once” saying quoted earlier. This fungus can actually be edible quite a few times before it poisons you. Unlike other toxins which you may expect to have a rapid onset after consumption (maybe a few days after ingestion at the most), the compounds responsible for the fatal poisonings attributed to P. involutus can take months to manifest. This is because the toxic effects often become apparent after repeated exposure, usually through the repeated consumption of the fungus. This is because the toxic compound here is in fact an antigen, which the body becomes sensitised to over time. Once enough meals of P. involutus have been eaten, the antigen present stimulates a rare autoimmune response where the body produces antibodies which attach to and disrupt red blood cells (autoimmune haemolytic anaemia). This causes life-threatening reductions in red blood cell counts, kidney damage and multi-organ failure. There is no antidote.
If in doubt…
So, there are three of the fungi that I find most interesting in terms of their toxicity. This only scratches the surface of the wild world that is mycotoxins – there are hundreds of others. From St Anthony’s Fire (a range of medieval diseases attributed to Ergot (Claviceps purpurea) to the near-certain fatality after consumption of Amanita phalloides or Amanita virosa (named the Death Cap and Destroying Angel respectively – foreboding!), mycotoxins are truly fascinating. These show the massive variety of toxins out there and how they influence both our health but our culture and relationship with wild foods. From a foraging perspective, the range of dangerous fungi out there clearly shows the importance of only foraging with an experienced guide and only collecting what you can identify with 100% confidence. If in doubt, leave it out!
NB from Girlymicro – Whilst we’re delving into some mycological (fungal) joy over a couple of blog posts I thought I would take the opportunity to re-share this four part article series on the fungi of The Last of Us, which was a real joy to be involved with, and a clinical article that may surprise you:
https://www.idtransmission.com/understanding/tlou-tales–episode-1-the-culprit-of-humanitys-downfall
https://www.idtransmission.com/understanding/tlou-tales–episode-2-the-devil-is-in-the-details
https://www.idtransmission.com/understanding/tlou-tales–episode-3-the-realities-of-the-last-of-us
https://www.idtransmission.com/understanding/tlou-tales–episode-4-living-with-the-living-dead
On a rather different note – sometimes people love their fungi just a little too much in other ways……….
All opinions in this blog are my own