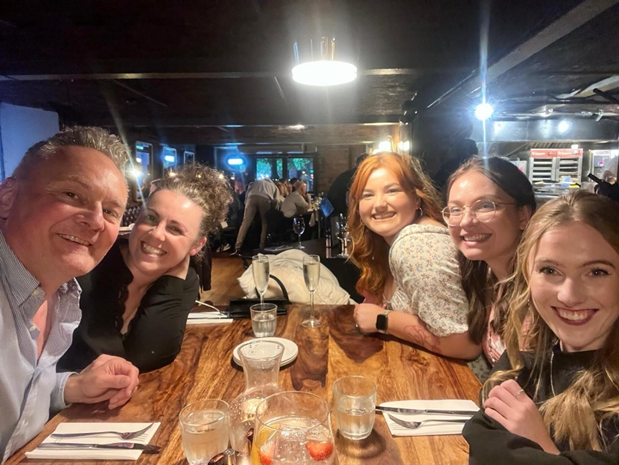This week has included some reflection for me on the importance of making our own luck. I’ve posted recently about both Tiara Syndrome and the Pygmalion Effect, which has made me think about what we can do to ensure that we are the main characters in our own stories, rather than drifting along. Being full blown participants in our lives, rather than falling into a trap of responding within rather than driving our tales. A key part of this is about how we respond to opportunities. How we decide to challenge ourselves by doing things that scare us. By choosing to step out of comfort and into the unknown. I’ve been thinking about how it is, that by consciously making small choices over and over again, we reach unexpected places and arrive at destinations we could never even picture when our journey began.
Last week I made one of those decisions, we actually it was before last week, but…details, the event was last week. In March, I noticed that there was a new series of events occurring in London pubs called Pints of Knowledge. The idea really resonated with me, it was the concept of bringing people who are interested in a really wide variety of topics into pubs, which are struggling right now, during the week and pairing them up with experts who are happy to sit and talk about a subject they love for an hour, and then hang around and answer questions. Now, as I have a policy of engaging with things that scare me and love an opportunity for learning and improvement, I threw my hat into the ring. That choice led me to trying something completely new last week, giving a public lecture in a pub on the subject of Infection in Movies and TV related to the book I’m currently working on.
Why was this different?
You will probably look at the above paragraph and say ‘what’s new’. You give lots of lectures, which is true, 1 or 2 a month on average. This was, however, a unique scenario that felt different. I have given lectures in pubs before, but not for ticketed events where people are paying money to hear what I have to say. I have given hundreds, if not thousands, of lectures before, but rarely to an audience of completely unknown backgrounds and interests. Even more significant, is that those lectures are rarely, if ever, linked to a really personal passion project, they tend to be more evidence based affairs. All of which made it a unique experience for me, and also required a certain level of vulnerability to be worked through. Something unknown, but something I deeply cared about doing well. This combination can make setting success criteria challenging, let alone delivering on those criteria.

No reputational protection
Having the words Professor in front of your name often provides a certain level of reputational protection. I’m usually asked to speak at events, and I generally work under the assumption that I have been asked either because they’ve heard me speak somewhere else and have decided I do an OK job, or because I know something about a specific, in my case likely very niche subject, that they want to hear more about. I don’t really have much to prove when I get up to speak, as someone has already made the assessment that I probably have something useful to say. Plus, when conferences have many streams, attendees could choose to go and listen to someone else if my stated learning objectives aren’t something they are interested in, so there is minimal risk for both myself and the audience.
Last week, I stood in front of a room of 80 people who frankly probably neither knew or cared who I was. They were there because the talk title interested them and they fancied a night out with a pint. Therefore, I felt like I really needed to earn my stripes and prove my right to stand on the stage and talk about something that I really enjoy, the combination of infection and movies and TV. When taking on a very different type of challenge, I know that if everything goes well, the high will be unreal. The counter is also true, there is at least some level of risk. In this case, risk that you aren’t the competent speaker you hope you are, and that you won’t be able to convey the topic in the awesome way it deserves. Therefore you won’t be able to deliver in the way that either you or the audience are hoping for. Going into the event, you have to be OK with accepting either outcome, as you will never truly know how the cards will fall until after the event.

No prior knowledge of the audience
As I’ve said, the tickets for these kinds of events are on general sale. You might, therefore, get movie lovers coming who don’t really know anything about infection. You might, and there were, get lots of scientists and people interested in infection in the audience, but this doesn’t guarantee that they will get your movie references. You may also get a group of people who have no particular interest in either subject area and just want a night out or a place for their next date. Deciding how you are going to structure your session, therefore, can be a little challenging. How much time do you spend on each section? How much intro to the film examples do you need? If you spend too much time covering areas people already know and understand, they are likely to get bored. If you don’t intro enough you’ll lose people and they may think you dull. All that before even considering whether your jokes will be funny.
It’s a unique experience talking in a public forum versus talking at a conference, or to a group of students, where you have some knowledge of the type of people who will be in the room. When you have that knowledge you can use it to inform putting together the story you want to tell during your presentation. Not having that starting info can, therefore, make things harder. It is however, a great opportunity to go back and undo some of the assumption you make during your normal talk structures and think how you could do it better by looking at everything through a fresh lens.
No learning outcomes
I mentioned learning outcomes before, and when I’m giving talks at conferences or in academic settings, I will always use learning objectives to guide expectations and offer sign posting to anyone attending. They allow people looking at agendas to really understand what my session is going to cover, and the pitch of the event, rather than just guessing based on titles. The interesting thing about doing a session like Pints of Knowledge is that it isn’t about continuous professional development, or walking away having addressed a specific learning objective. My main objective was to deliver a session in a way that was entertaining and allowed people to have a good evening, with walking away having learnt ‘facts’ as a secondary outcome. It’s about opening the door to a topic so that anyone interested can then feel like they have a starting point to access more info if the session speaks to them. To me, you are acting as a guide not a teacher, and that means that whether a session is ‘successful’ probably is something different than ticking off a number of topic points discussed.
Pitching considerations
Having spoken about the fact that you don’t have any prior knowledge of your audience, pitching can be challenging. This includes not just the structural components I’ve already talked about, but how you pitch your content. What kind of language do you use, which words and terms do you need to explain. Pitch too high and you will lose people, pitch too low and people will feel talked down to. One of the great things about these events is that they are in person. This means you have the opportunity to hear how people are talking to each other before the session starts and what they say they are interested in, when no one knows who you are. You can also see their faces and reactions as you are the giving the session, which allows you to react and adjust your content in the moment. This is one of the reasons that I tend to use text light slides when I’m speaking to audiences that may be mixed, or I know less about. This enables me to adjust my content in the moment, spending more time explaining if needed, or expanding on things the audience are responding to more. It can take a chunk of self confidence to stand there and know that you are going to try and read the room and respond, but when the pitch is uncertain it may be the best way to ensure everyone is having a good time.

Facing up to the unknown
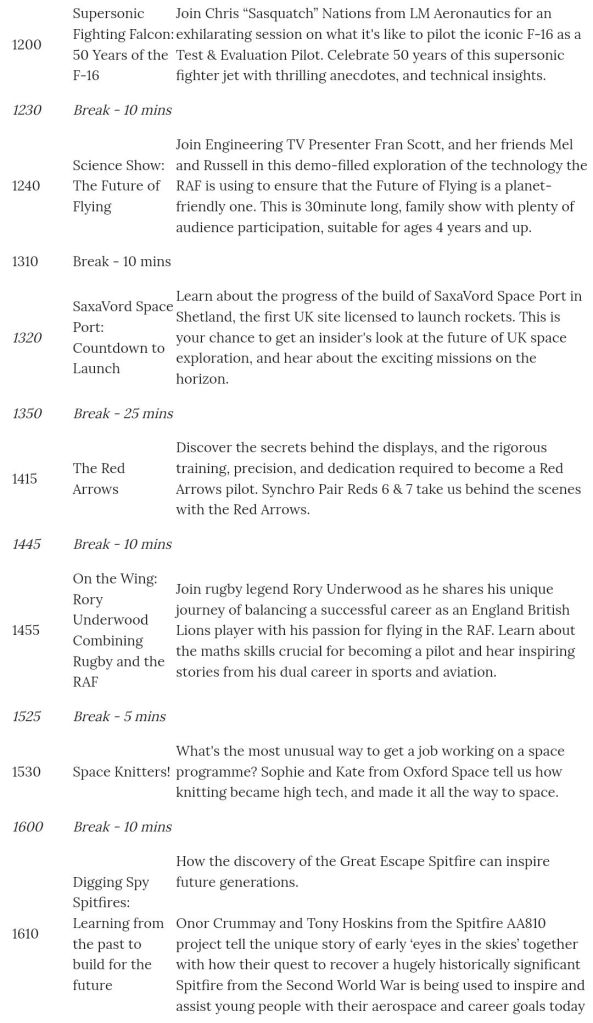
The other facet to this is that the organisers don’t know you either. They have taken a chance on you, and if you are anything like me, you want to show them that that risk taking is warranted. If I’m organising an event, I will usually know the venue. I will know how many seats there are. I will know how many tickets I have sold. For this kind of event you have none of that information. The screen shot below was taken when it came up on my feed after the event. I spent most of the run up terrified that no one would be interested enough to buy a ticket, the organisers would be disappointed, and that would have an impact on something that I think is a really great endeavour. There is a responsibility that comes to something like this.
Being OK with having less control than you would normally have is key to stepping out of your comfort zone, irrespective of activity. Stepping out is a key component of learning and improving, and so it is important we acknowledge that discomfort is just part of the process. Let’s not fight it, let’s just accept it.

Wearing your heart on your sleeve
All of this sounds simple…right? The logical part of my brain always thinks so. That’s why I sign up for these things. We are however all more than logic. We are whole individuals with an emotional component to what we do and how we react to things. So despite my logical brain saying, ‘I’ve got this’ the feral emotional part of my brain can easily spiral. This is especially true when I really care about something I’ve committed to.
In this case it was a session on topics I love so much that I’ve committed to writing 80,000 words about them. The fear of standing up and saying this is something I love, this is something I find fascinating, and seeing a room full of faces that look back with skepticism, or worst still boredom, is not something that is easy to shake off. Acknowledging that our responses, or at least mine, are never going to be entirely seated in logic is an important part of managing the fear that stepping into the unknown and challenging ourselves can create. Instead of asking ‘why do I feel this way’ and stopping there, following on with acknowledging that feeling and working with it, rather than ignoring it, helps me at least get out of my own way.

So what practical things can you do to find a way through the fear?
Preparation is key
The first thing is to do your research. There will be unknowns that you can’t address, but there will be ones that you can, in order to remove some of questions about what is expected.
For Pints of Knowledge, they were kind enough to give me a free ticket so I could attend a session from someone else. Now, that session was in a different venue, with a very different topic, but it let me get a feeling for the vibe and what kind of people might make up the audience. It also let me understand what kind of talk structure other people were using, the types of questions that the audience might ask, and the way the speaker responded to them.
I also spent a lot of time talking to people to see what they might be interested in if they were going to see a talk with a similar title. What terms were people used to, what terms might require a little more explanation? Mr Girlymicro also put up with me talking about, running concepts, and hearing the presentation, during the run up. One of my brilliant IPC team, who isn’t a big movie fan, even agreed to hear a full run through and then gave me feedback on how well it landed for someone who was interested in one component, but not so interested in the other. You can’t do much about the true unknowns, but you can work to address the unknowns that may have solutions if you decide to put in the work in advance.

Focus on your audience
This is probably not revolutionary, but it is something that took a while to really land as a piece of my thinking and prep when I started speaking at sessions more regularly. It’s not about you. As someone invited into a space to give a session, you are a guest in that space, and it shouldn’t be about you and what you want to deliver, it is about the audience. What might they find interesting? What might they find entertaining? If you are talking linked to a learning event, what might it help them to learn in a way that works for them? What pieces of knowledge would help them achieve the goal that led them to attend? I find this shift in perspective really helps. It also pushes me to be more inventive in my approaches. It also can prevent me being stuck in my own head, or getting caught in a loop linked to aiming for perfection. What I want to achieve is likely different from my audience, and shifting my focus and success criteria to centre on them, stops me tying myself into knots trying to achieving 2 things simultaneously that may have different requirements.

Ground yourself in what you know
The other thing I find helpful, if I’m nervous or unsure, is that I walk the right line in terms of pushing myself in some aspects but not in all areas at the same time. If you are speaking to a new audience, or ones where there are lot of unknowns, then it is best to ground yourself by talking about content that you are familiar with and confident about. If you are speaking to an audience you know well, with less unknowns, then you can probably take risks and push yourself in terms of content and content type. When I talk about stepping out of your comfort zone, I think there’s a difference between pushing your boundaries and stepping into something new, versus taking a giant leap into an arena that is completely new in all aspects. I’m not saying you can’t do that, but if you are doing something to develop or expand learning, I find it beneficial to expand on a previous skill or knowledge set, rather than trying to do everything at once. If things don’t work out and it’s all new, it’s hard to know which aspect had the greatest impact on whether it succeeded or failed. That means it is harder to develop a plan to address the any development gaps. Development is iterative, and so taking a step wise approach can benefit you in terms of both managing any anxiety or fear, as well as in guiding what a development plan might look like.

Be OK with ‘what’s the worst that can happen?’
I’ve written before about the Rule of Thirds. The fact that 1/3 of people are likely to love something you create. A a third of people are likely to be ambivalent, and a third of people are likely to have a variable level of negative opinion. If you manage to shift those numbers towards the positive you are doing amazingly well, but don’t ever be deluded enough to think you will have 100% positive result. You can’t impact the mood someone was in when they sat down to listen to you, or the fact that someone got stood up or arrived late and it’s put them in a humph. Someone’s mood will impact how they feel in the space and how they interact with your offering. There’s not much you can do about that, so sometimes you can give the best session in the world and an individual is going to still have a sucky time.
All of which brings me to the question I ask myself when I spiral ‘what’s the worst that can happen? If I give a bad talk then I probably won’t get invited back. Will that be the end of my career? No. Will that mean people won’t buy my new book? Maybe, but also I’m not writing my new book to become a millionaire, I’m writing it because I think it’s something others might be interested in and to share a topic I love. The number of copies sold is a very minor part of my success criteria. Will my ego take a knock if it goes badly? Yes, but that’s ego. It won’t be the first time I’ve had a set back, and every set back has led me to go back to the drawing board and to learn how to be better, so really each has ended up being an opportunity.
The main thing is to be honest with yourself about the consequences of stepping out of your comfort zone, put it into context, and make an informed decision whether this is something you want to do. Most important of all, once you have made that decision in a calm and logical place, stick to it. Don’t let later emotions overwhelm your decision making. Acknowledge how you feel but don’t be driven by the fear response.

The pay off is worth the risk
If nothing else, when you feel the wobble, when you ask yourself why you decided to do this, re-focus and remember the reason why you said yes in the first place. Remember what you were trying to achieve, and keep that vision in front of you to remind yourself of where you are trying to get to.
I was pretty terrified before I got up on that stage. My self doubt ran wild. I still got up and did it. It reminded me of why going through the fear was worth it. Not only did the session seem to go pretty well, but I answered questions for an hour and half, and met some really wonderful people that I would not have met otherwise. I saw friends and family come together to support me, and it was lovely to have an event where they could turn up and see what I do as part of the day job.
Like always, you will get far more out of stepping into the unknown that you had predicted. There will be unexpected payoffs and bonuses that you couldn’t have foreseen. Even without that though, you will have taken steps to develop yourself and build confidence that will make you even braver when making your next decision. The unknown should be less of a place of fear, and more considered a world of opportunity. If we take steps into it regularly enough, we remind ourselves of the benefits that taking steps outside of our comfort zone hold.
All opinions in this blog are my own
In case you’d like to see them, these are the slides I used, and if it’s of enough interest to people I may even record the session and put it up on my YouTube channel – let me know if you’re interested. Also, a massive thank you shout out to Steve Cross for the photographs. Steve does a number of creative things, public engagement, consultancy, and comedy sessions, as well as photography so if you are interested give him a shout.