I’ve been fortunate enough to have spent pretty much my whole career working in paediatrics (children’s medicine) and I’ve already written about why this is so important to me. What I haven’t really talked about before is the thought process that I often encounter out in the real world i.e. that there isn’t really much of a difference between infection prevention and control in adult and paediatric settings.
To really get some of my thinking straight about this I’ve just finished writing 4 hours of lectures on paediatric infection prevention and control. You may be reading this and thinking that this seems like a bit of waste of time as surely the principles of IPC are universal, stop the patient getting infected right? Well yes and no. The principles are the same, as you can see from the picture below, but the challenges, organisms and therefore final risk assessments aren’t (see my previous post on risk assessment here). On a higher level things might look similar but when you get into the detail children and young people are different from their adult counter parts and so we need to make sure what we’re doing meets their needs, rather than giving them the best fit we can manage.
For those you not interested in paediatrics I’m hoping this will just help support thinking on taking a one size fits all approach in any setting and how appropriate (or not) it might actually be.
The organisms that challenge us are different
Many of the organisms that are the focus of mandatory reporting because they cause such a lot of issues for adult patients are not the same organisms that cause most difficulties within the paediatric setting. Two really good examples of this are MRSA bacteraemias and C. difficile. Unlike adult settings I may report a handful of MRSA bacteraemias a year and up to 40% of the under 2’s may be colonised with C. difficile but don’t display any symptoms or go on to develop infection. Therefore these benchmarks are not particularly useful for driving improvements in paediatric settings.
That’s not to say that line related infections are not a problem, paediatric patients are much more likely to interact with lines, play with them, suck on them, pull them out. The lines themselves may also need to be placed in non ideal sites – such as femoral lines in a patient whose nappy wearing, just because of difficulties in getting access. This means that Gram negative line infections, skin flora and yeast may be be more of an issue in these patients depending on the source.
The big thing to bear in mind though is that viruses, both respiratory and gastric, are probably the biggest transmission challenge. Children acquiring viral infections for the first time shed very high loads and often cannot communicate their initial symptoms. This can be compounded by the fact that children may also asymptomatically shed viruses and therefore have no symptoms at all in order to drive specimen collection. Other viruses, such as chickenpox, are infectious prior to the development of symptoms and therefore unless prior exposure to the patient is already known, it may be impossible to prevent exposures to others.
Exposure levels are different
I’ve already mentioned that children may excrete higher levels of viruses when experiencing primary infection (1st infection) versus reinfections, like we experience as adults or in older children. Therefore the level of virus that other patients are exposed to is likely to be higher.
The other thing is that in a specialist paediatric hospital patients may stay for prolonged periods of time or have many repeat visits – leading to not just a one off exposure but cumulative exposure over time. This cumulative exposure increases the chance that a patient will become colonised or infected, it’s all about % conversion chance after each encounter. The risks in a specialist paediatric centre are therefore very different.
The exposure risks don’t just come from other patients however, we’ll talk about staff and carers later, but there are also environmental exposures. Extended amounts of time in hospital expose patients to the healthcare environment in a different way to a single short stay. Risks from equipment linked to water, and therefore opportunistic pathogens, are greater in long stay complex patients. Patient factors that mean they need to stay in specialist mechanically ventilated room are also different in this patient group. The need to monitor and control these factors is therefore really important (check out the Environment Network if you want to hear more about this).

The underlying conditions are different
Working in a tertiary referral centre (specialist children’s hospital) many of the patients we support have complex conditions or are acutely unwell. I’ve already talked about the fact that this may mean that cumulative exposure becomes more of an issue due to prolonged length of stay. There are other things however that mean that they may also be at higher risk of infection. The nature of their condition may mean they have lots of lines and/or skin breaches, meaning they have gaps in the bodies natural protection systems. They are also likely to be on lot of different medications that may cause immunosuppression or in the case of antibiotics, impact on what microbes they have on board. These things will change their risk just by changing what’s going on within their bodies. The more different medications and the longer they are received them, the greater the risk that needs managing.
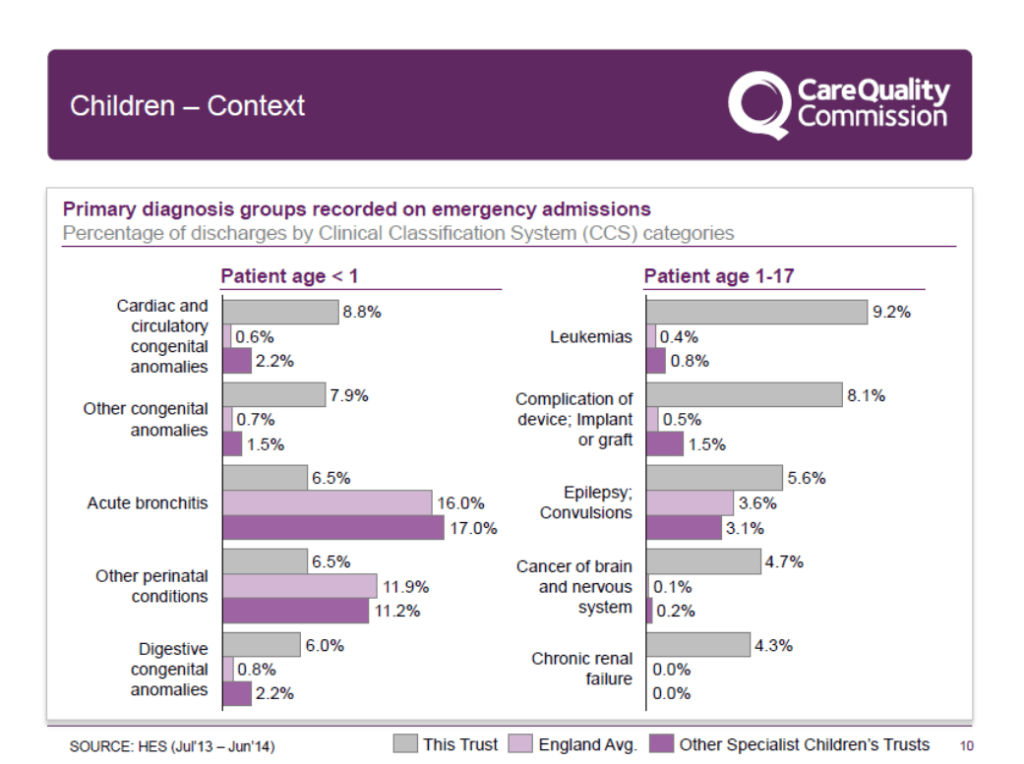
One other thing to bear in mind is that paediatric patients get admitted with different conditions to their adult counterparts. There are even differences between the different age groups within paediatrics about how they present. You can see the under 1’s present differently from the overs 1’s, once you start getting over 12 the presentations may start to look very similar to those of young adults and so are different again.
The ways patient interact with their own bodies and the things around them is different
So we’ve established that the microbes these patients have are different and that the very things we do to help these patients recover may also impact on their risk of infection. Children are also different in the way that they interact with both their own bodies and the rest of the world.
I’ve been a hospitalised child myself and when I was in intensive care I apparently spent a chunk of time pulling out my lines when I was semi sedated. I’ve had patients who knew the world would come running if they sprayed blood from their Hickman line. Then there are the patients where you’ve had to put (femoral) lines into the artery in their thigh as its the only place where you can get access, but the patient is also wearing nappies and we know that nappies can leak. All of these things can make the line site which is supposed to be kept clean and with limited interactions challenging to maintain in children. The same is true for other plastics and objects that are there and breach the bodies natural defences. They may therefore get organisms from sources that adults are less likely to and these interactions are important to identify when undertaking your risk assessment so that you can take different actions to prevent them from happening.

Interactions with other people are also different for children. When a baby is distressed in hospital, staff as well as carers will pick up and sooth them. Paediatric patients therefore may have prolonged close physical contact with the staff on wards in a way that patients may not in an adult hospital. There is a risk therefore of picking up infections that may have mild presentations in adults but which may be more severe in children, such as whooping cough.
In Trusts like mine where parents stay on site as main carers for their children, there are also a number of considerations linked to infectious transmission to and from carers to their children. This has been a really key consideration during the COVID-19 pandemic where we considered children and their carers a bubble whilst on site. In these scenarios where family are supporting in care provision it can be challenging. Your first line of advice would always be for symptomatic carers to stay away but that isn’t always possible. In a scenario where the infection is transmissible for 48 hours prior to symptom onset then the child has often already been exposed and therefore its about what happens to further reduce risk. Sometimes carers will have to leave site, especially if they are unwell enough to require support themselves, in other cases interventions such as them wearing a mask may reduce the risk enough. Managing the risk benefit equation in these scenarios is something that is probably experienced most in paediatric settings.

One of the other big differences is the way that children interact with their wider environments. Patients with me for a long time will be learning to crawl or walk within their environments, they will therefore be grasping for things and interacting the floor in a different way. Other children will be playing with items on play mats that are by their very nature near the floor. When they throw things (as children do) they may sometimes try to retrieve them and therefore touch the area outside of that mat. I’ve also had many patients in that developmental phase where they will put anything in their mouths, including shoes and anything else within reach. This interaction with the environment is key to development but obviously brings with it extra issues and risks that need to be controlled within the healthcare setting.
Finally in this section I want to talk about toys. Toys and play are essential to development, in fact there the RCN is due to launch some guidance on this later this year that I was involved in developing. Play is super important and can also be key in healthcare to supporting interactions and limiting distress. The right toys and understanding the risks that different types of toys and play interactions bring is a key part of risk management. Wet play for instance is not something that most hospitals would recommend. It’s OK to give out a teddy bear that a patient will take home but not to have one that goes between patients. Books and jigsaws are a no no as unless made of vinyl or plastic they can’t be cleaned properly in between patients. Each toy needs to be thought of separately and decisions made about where it might be most appropriate.
Interventions are different
Some of the interventions we need to think about in paediatrics may therefore be different to adults in terms of managing the slightly different risks. For instance having age appropriate boxes of toys that can be cleaned between patients is the kind of approach that can be undertaken so as to maintain access whilst still limiting risk.
Standard IPC interventions, such as isolation, need to be thought about carefully in paediatric settings. Isolation can impact on developmental milestones as patients will see fewer people and therefore have significantly less access to interactions to support speech and communication development. The balance of this is that if a patient acquires an organism, because others weren’t isolated appropriately, then they will likely carry that organism for a period of years and so the consequences of getting things wrong can impact patients for years
It’s a family affair
One of the key things to remember about paediatric settings is that when you are looking after children you are almost always going to be looking after their families too, in terms of emotional well being at least. When you are putting a child in isolation you are also isolating their carer. This means that at a time of usually heightened stress we are removing a parent from their support network also, sometimes for months at a time. It’s important therefore that we take the time to get to know them as people as well as carers for our patients. I’m as guilty as anyone of calling people ‘mum of XX’ instead of a name. This may have less of an impact if its for 2 days but when you are looking after your child away from other support then losing your name is just another step towards losing your identity. I’ve included the link to a twitter thread here which discusses a little bit about what it’s like to be on the other side of this particular table which I found to be an important reminder.

I hope you’ll agree that working with children is a privilege. To provide the very best in care to this patient group we need to view them as people in their own rights, they deserve us taking the time to think about them and their needs, in a way that is potentially different from other more adult focussed settings.
Anyway, here is the talk that finally came out of the ruminating on this topic, hopefully it might be useful to some of you.
All opinions on this blog are my own


[…] that just wasn’t true, at least within the paediatric environment. I’ve written just recently about why paediatric IPC is different and the environment and the way that patients interact with […]
LikeLike
[…] posts I’ve done on risk assessment including the post the podcast above refers to, one on paediatric risks and one on environmental […]
LikeLike